
Cough and chest tightness mistaken for pneumonia? A stem cell transplant combined with CAR-T therapy brings him back from the brink of life
Recently, Mr. Wu (not his real name) returned to Sir Run Run Shaw Hospital (SRRSH), affiliated with Zhejiang University School of Medicine, for a follow-up examination, with all indicators showing positive results. Accompanied by his wife, he strolled down the hospital corridor with a light step. It is hard to imagine that over the past year and a half, he and his family endured an incredibly difficult period, as an aggressive lymphoma pushed him to the edge of life and death on several occasions. Fortunately, thanks to the dedicated efforts of the medical team led by Senior Consultant Dr. Xiao Haowen and Consultant Dr. Jiang Hao from the Department of Hematology and Cell Therapy at the Grand Canal Campus of SRRSH, Mr. Wu navigated through multiple rounds of chemotherapy, an autologous hematopoietic stem cell transplant combined with CAR-T cell therapy. He ultimately overcame numerous critical challenges and regained a new lease on life.
Mr. Wu, 58, lived a simple, stable, and happy life with his wife and son. This tranquility was completely shattered in September 2024. He initially visited the Department of Pulmonary and Critical Care Medicine at SRRSH due to a cough accompanied by chest tightness and fatigue. After admission, he developed recurrent high fevers along with pancytopenia (a decrease in all three blood cell lines). Following a consultation with the hematology department and further examinations, doctors discovered multiple enlarged lymph nodes in Mr. Wu's neck and armpits, as well as an enlarged spleen. Blood tests revealed very high ferritin levels, and a bone marrow examination found hemophagocytic cells – indicators of hemophagocytic lymphohistiocytosis (HLH).
To establish a definitive diagnosis, a lymph node biopsy was performed on Mr. Wu’s right collarbone area. The pathology result indicated “diffuse large B-cell lymphoma" (DLBCL). He was ultimately diagnosed with "non-hodgkin lymphoma, diffuse large B-cell lymphoma complicated by hemophagocytic lymphohistiocytosis (HLH)." A PET/CT scan revealed even more distressing news: lymphoma lesions had involved multiple sites throughout his body, including lymph nodes, the spleen, and several bones (Figure 1). Lymphoma complicated by HLH is clinically a very aggressive and dangerous condition with an extremely high early mortality rate. This diagnosis was undoubtedly a bolt from the blue for Mr. Wu and his entire family.
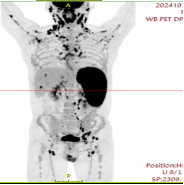
Figure 1
The team led by Dr. Jiang Hao promptly developed and implemented a targeted treatment plan for Mr. Wu. After several cycles of chemotherapy, not only did Mr. Wu's life-threatening condition stabilize, but his lymphoma also achieved complete remission (CR). His physical condition essentially returned to its pre-illness level, bringing immense joy to him and his family. Considering Mr. Wu's initial presentation complicated by HLH and his high risk of relapse, Dr. Jiang Hao recommended an autologous hematopoietic stem cell transplantation (auto-HSCT) as consolidation therapy. However, Mr. Wu and his family, very satisfied with the results of the initial chemotherapy, did not adopt this recommendation at the time.
Sudden Relapse After Initial Remission
Unfortunately, less than four months after his last chemotherapy session, in June 2025, a mass reappeared in Mr. Wu's neck. It continued to grow and was accompanied by ow-grade fevers. He immediately returned to SRRSH and sought out Dr. Jiang Hao. A repeat biopsy of the neck mass was performed, and the pathology result again confirmed "diffuse large B-cell lymphoma." Genetic testing further revealed a 51% deletion rate of p53 gene. Further investigations showed that lymphoma cells accounted for a staggering 20% of his blood cells. A PET/CT scan also indicated that the number and extent of lymphoma lesions were more severe than during the initial diagnosis (Figure 2). This meant Mr. Wu's lymphoma was an early relapse, significantly more dangerous than his first illness episode. The aggressive nature of the recurrence, resistant to conventional chemotherapy drugs for long-term control, plunged him and his family into deep despair again.
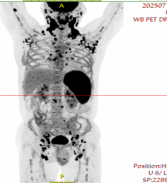
Figure 2
Treatment Decisions for High-Risk Relapse
Dr. Jiang Hao conducted a detailed analysis of Mr. Wu's condition: his DLBCL had relapsed early, complicated by a p53 gene deletion, and had previously been associated with HLH – all factors classifying him as a high-risk case. Based on this, Dr. Jiang Hao strongly advised Mr. Wu to undergo chemotherapy followed by an auto-HSCT as soon as possible. To achieve a more durable remission, he recommended combining CAR-T cell therapy with the transplant.
Complete Remission Following Combined Cellular Therapy
After discussing with his family, Mr. Wu decided to proceed with the auto-HSCT combined with CAR-T therapy. The teams of Dr. Xiao Haowen and Dr. Jiang Hao from the Department of Hematology and Cell Therapy jointly developed a comprehensive treatment plan for him. In late July 2025, Mr. Wu underwent T-cell collection (apheresis), followed by the manufacturing of his CAR-T cells. He then received a new round of chemotherapy. After just one cycle, follow-up examinations showed significant shrinkage of his lymph nodes, and lymphoma cells in his bone marrow had disappeared. In early September 2025, sufficient autologous peripheral blood stem cells were successfully collected from Mr. Wu. By mid-September 2025, he entered the transplant unit, received pre-transplant conditioning chemotherapy, and subsequently received infusions of his autologous hematopoietic stem cells and his CAR-T cells.
During his more than one month in the transplant unit, Mr. Wu faced numerous severe challenges, including critical infections, gastrointestinal bleeding, and Cytokine Release Syndrome (CRS). With the full support of Dr. Xiao and Dr. Jiang's medical teams and the meticulous, expert nursing care provided by Head Nurse Shen Yazhou's team, Mr. Wu successfully achieved hematopoietic reconstitution and was discharged from the unit (Figure 3). On December 29, 2025, Mr. Wu was readmitted for a follow-up examination, which confirmed his lymphoma remained in complete metabolic remission (CMR) (Figure 4). During this pre-New Year check-up, his indicators showed continued improvement, and he had even gained some weight. This renewed lease on life prompted him to express his sincere gratitude to the medical and nursing teams of the Department of Hematology and Cell Therapy at the Grand Canal Campus of SRRSH.

Figure 3
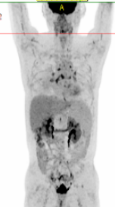
Figure 4
The SRRSH Team: Safeguarding Patients with Blood Disorders
The Department of Hematology and Cell Therapy, which successfully treated Mr. Wu, is a specialized platform combining the Integrated Diagnosis and Treatment Center for Malignant Hematologic Diseases, the Hematopoietic Stem Cell Transplantation Center, and the Cell Therapy Center. The department offers multiple cutting-edge cellular therapies, including hematopoietic stem cell transplantation, CAR-T cell therapy, cord blood stem cell therapy, and mesenchymal stem cell therapy. This allows them to tailor individualized treatment plans based on each patient’s specific condition, significantly improving survival rates and quality of life. Moving forward, the department will focus on advancing innovation in cellular therapy technologies, aiming to provide more patients with blood disorders greater choices and hope through more refined, cutting-edge techniques and superior patient care.















